Occasionally, we are fortunate to have a moment of inspiration that changes the way we view a problem that we are facing. For me, this moment happened at the intersection of third grade engineering and lip filler. I have been injecting dermal fillers for eight years and, like most of you, my first passion was injecting lips with dermal fillers. I eagerly soaked up any mention of better ways to create the perfect lip. I would pore over photos that other injectors posted and try to understand how they accomplished their results. I tracked down the source behind every mention of new, innovative lip filler techniques. I even paid serious money to watch some of the world’s best injectors inject and would hound them for clues on how to become a better injector. The more I researched, the more I became stumped. I kept recognizing a certain pattern in the shape of lips that for the life of me I could not figure out how to correct.
The Dilemma
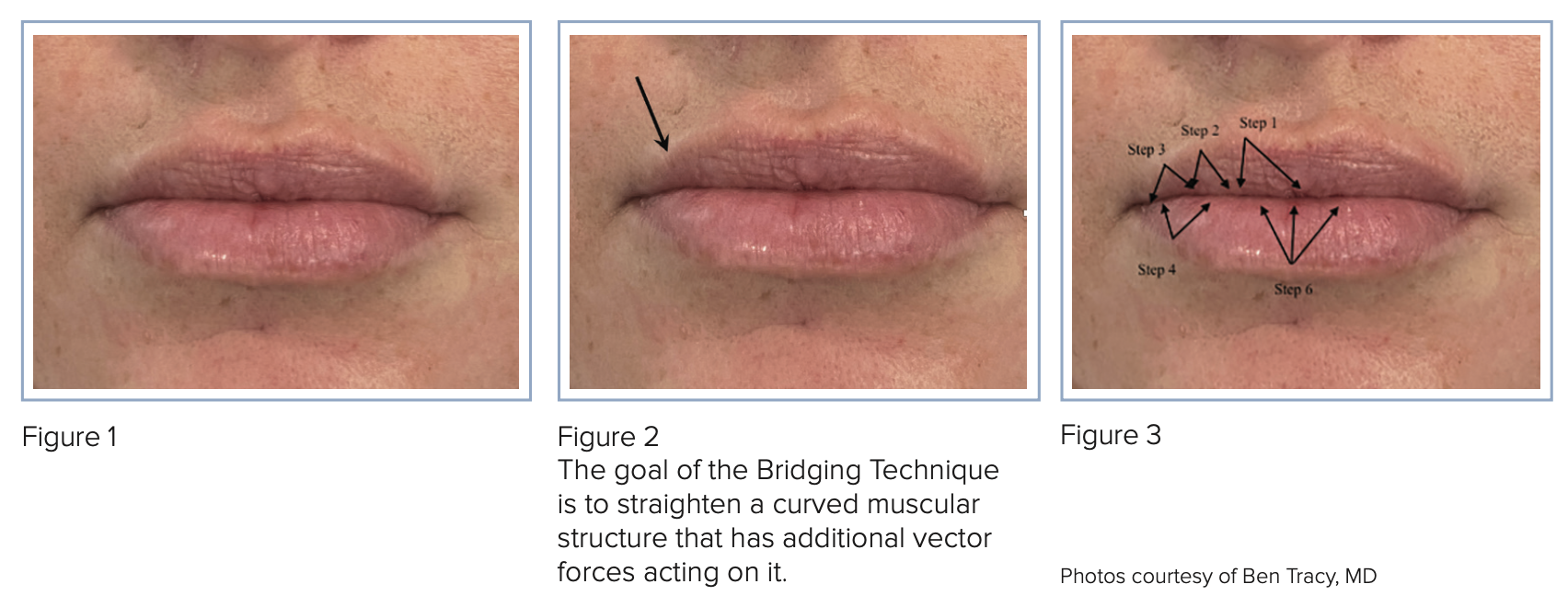
I want you to take a moment and analyze the lips in Figure 1. When I have taught this live some of the first things people note are:
- She has asymmetry left to right with her left more pronounced
- Her Glogau-Klein (GK) point is more crisp on the left
- She has volume loss with evident wrinkling in the top lip
- Her bottom lip is larger on her left
- She has large lower lip tubercles, large top lateral tubercles and a small top central one
- The oral commissure on the right is more downturned
These are all perfectly true observations and things that we need to be aware of when we are injecting lips with dermal filler. But the thing that jumps out to me is what the lip does just medial to the oral commissure, which is most prominent in this case on her right side. The lip starts to buckle over itself as we approach the oral commissure. This tends to happen more significantly on one side and with classic lip filler injection techniques we often end up exacerbating the problem.
Lips are a highly mobile structure that gain their shape and volume from the orbicularis orismuscle. Also known as the musculus orbicularis oris, the orbicularis oris muscle is a complex, multi-layered muscle that attaches to the dermis of the upper and lower lip through a thin, superficial musculoaponeurotic system. It also serves as an attachment site for many other facial muscles around the oral region. One of its functions is to act as a sphincter around the mouth.
Using a soft hyaluronic acid (HA) dermal filler, the end goal is to straighten a curved muscular structure that has additional vector forces acting on it (Figure 2). There are two clinical pearls that can be drawn from the anatomy to help you achieve this. First, we are trying to create a straight line within a curved structure. One of the common goals of lip filler injections is to create a straight line at the wet to dry border at both rest and with animation. Second, there are many competing muscular forces in the lip tissue. My general philosophy is that muscles are always going to win in a battle of force against HA dermal fillers.
The Solution
I was able to find the solution for my lip filler dilemma when observing my son’s school project where the goal was to make a bridge structure and to see which design from each classmate can hold the most weight.
I took this concept back to my practice and with a patient’s approval, I was able to put it to the test. We found this theory actually worked very well in practice. The reasons why are actually pretty simple and have been known in structural engineering and architecture for centuries.
When you place a force straight down into the lips with a post or pillar of dermal filler you achieve a compressive force along that filler line and then to either side there is a tension force that has a displacement in the opposite direction. This causes the tissue to have increased buckling, which exacerbates the problem. What happens when you place that pillar or post at an angle instead of straight, is you still get a compressive force along the pillar or post of dermal filler, but now the tension force is actually displaced laterally. And that is the secret – the laterally-displaced tensile force creates a straight line.
My Bridging Technique (see Figure 3)
Step 1: I start from the GK point of the cupid’s bow right at the pink mucosa and take into account the size, shape and location of the top lip tubercles. I will then “bridge” the tubercles with angled threads at a depth that correlates to the properties of the dermal filler I am using, always staying above the muscle. The angle somewhat depends on anatomy, but the goal would be 45°. I do not inject into the tubercles directly. At the wet to dry junction, I will do a small bolus of dermal filler and then through retrograde injection create the actual pillar of filler. I bring the pillar close to my insertion site and without exiting I redirect the needle 45° in the other direction and create the second angled pillar. This second pillar I continue all the way out of the insertion point, leaving a drop on the exterior of the pink lip. From each injection insertion point, I create two angled pillars that bridge the area of concern. The volume of the bolus and pillars depends on the overall anatomy and correction needed for symmetry and fullness.
Step 2: I move lateral to reach roughly the halfway point to the oral commissure that allows for me to create another set of 45° angled pillars that start at the wet to dry border with a small bolus. Then in retrodgrade fashion, I create the pillar as in step 1.
Step 3: I start right above the buckling point that is just medial to the oral commissure and create two more pillars of filler that bridge the buckled tissue on either side at roughly the same 45° angle. This means that one side of the top lip is done.
Step 4: I then proceed to the lower lip on the same side and choose a single insertion point that will allow my 45° angled pillar to end just medially to the oral commissure in one direction and just lateral to the tubercles in the other. Using the same process, I create both of the angled pillars from the single injection site.
Step 5: I then move to the center line of the lower lip between the two bottom pillars and instead of creating two angled pillars, I create pillars in a “W” shape to create medial fullness, volume, curvature and pout. I again avoid the tubercles and have the two lateral injection pillars stay on the medial borders of the tubercles and the third pillar stay midline.
Step 6: Repeat steps 1-5 on the second side. This is the Bridging Technique in its most basic form that I have found creates a beautiful outcome and high patient satisfaction, with a reduction in quantity of pokes and adverse events. But in my mind, this is a technique that is meant to be further explored.
With an understanding of the concept of the Bridging Technique I hope that this inspires someone to take the next step forward and continue to create and expand on how we do our aesthetic treatments.
About the Author Ben Tracy, MD
Ben Tracy, MD
Dr. Tracy is a master trainer and medspa advisory board member for Allergan. In addition to this Bridging Technique, he is the creator of the “Suspended Thread Lift”, “Fluid Face Lift”, “Fox Tox Eye” and more. He has been married to his beautiful wife for 20 years and together they have four boys and one little princess. When not holding a syringe, he enjoys exploring new destinations, eating culinary delights, and working towards healthier living.

